Resources
Welcome to the Verathon resource center where you can find more information regarding product training and industry news.
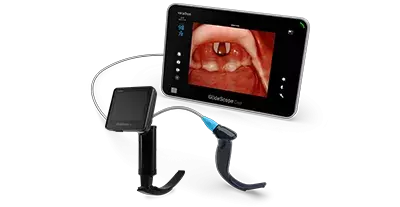
Airway Management
Explore training resources and industry news on airway management, video laryngoscopy, and Verathon's Total Airway Solution™.
Bronchoscopy
Explore our training resources for Verathon BFlex bronchoscopes and stay updated with the latest bronchoscopy industry news.
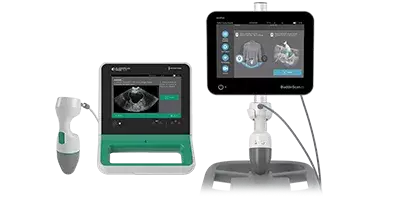
Bladder Scanning
Access helpful training videos for BladderScan products and stay updated with the latest bladder management industry news.
Featured Videos

Glidescope Go2 EMS Eagle County Paramedic Services Testimonial
Eagle County Paramedic Services has integrated the GlideScope Go 2
Total Airway Solution™ Testimonial
Single-use Video Laryngoscopy and Bronchoscopy in One

BladderScan i10 Probe Drop Test
Demonstrating MIL-STD-810H testing of the BladderScan i10 probe
Landmark Video
Laryngoscopy Study
Trial published in the Journal of American Medical Association concluded that GlideScope® hyperangulated video laryngoscopy outperformed direct laryngoscopy for endotracheal intubation in the operating room.
Clinical Publications

Video Laryngoscopy vs Direct Laryngoscopy for Endotracheal Intubation in the Operating Room
Cluster Randomized Clinical Trial

Performing Bronchoscopy in Times of the COVID-19
These recommendations for physicians who perform bronchoscopy will help to protect those patients...
Evaluation of the BladderScan® in estimating bladder volume in patients
To evaluate the reliability of estimates of bladder volume (BV) in children...
Need help?
Visit our Service and Support page for product documentation, repair requests, and to contact our dedicated customer service team via phone or email.