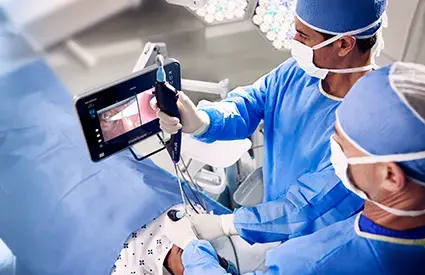
When the first ultrasound bladder scanners were introduced over 30 years ago, the ability for nursing staff to make non-invasive urinary bladder volume measurements became a valuable tool in catheterization decisions, management of lower urinary tract symptoms (LUTS), monitoring post-operative and post-partum urinary retention (POUR, PUR), and bladder training.
Today’s bladder scanners are far more technologically advanced. They can more accurately guide the clinician and compensate for human factors in usage and for variables in the patient. The latest technology simplifies and streamlines workflows and reduces operating costs.
As technology progressed, some myths have developed around bladder scanner usage and technology. This article will dispel the most common of these myths, so you can make a clear choice when it comes time for your next equipment investment.
Myth #1:
CAUTI Is under Control
Myth #2:
The Latest Consumer Technology Is the Greatest
Myth #3:
Accuracy Is an Easy Number
Myth #4:
Artificial Intelligence Replaces Skill
Myth #5:
I’m Worry Free With a Warranty
___________________________________
Myth #1:
CAUTI Is under Control

CAUTIs cost up to $8,700 per infection7
Unfortunately, urinary catheters are not always placed for appropriate indications nor are some care providers even aware of their presence in patients they are treating. This leads to unnecessary and often prolonged catheter use and increased risk of a catheter-associated urinary tract infection (CAUTI).1
CAUTI causes delays in recovery, increased costs associated with hospital stays, and may even result in death.2 After some early lack of progress, there have been steady declines in CAUTIs over the past few years.3 However, studies show it remains a stubborn concern.4
The key is that CAUTI is largely preventable. Bladder scanner technology reduces unnecessary catheterization by nearly 50%5, lowering the risk of infection. And in one major Southern California healthcare system, the use of bladder scanners in the emergency department reduced the use of catheters by up to 80%.6
Bladder scanners are an important investment consideration for your medical practice. Beyond providing equipment, your bladder scanner vendor should be able to partner with you for 1) staff training, 2) product lifecycle planning, and 3) clinical adoption and optimization.
Your bladder scanner vendor should also provide you with ongoing onsite assistance to help you achieve your objectives around infection control compliance and improved patient outcomes.
Myth #2:
The Latest Consumer Technology Is the Greatest

In recent years, many consumer devices, like smartphones and tablet computers, have made their way onto the hospital floor. These technology tools have become essential for accessing patient digital records, analyzing diagnostic results, and communicating between providers. But there are key differences between the daily use of these consumer devices compared to bladder scanners.
A bladder scanner is exposed to pathogens during patient contact with the ultrasound probe. Pathogens can also be transferred to a touch screen when the user is operating the device. To avoid risk to the patient, the entire system should be resilient to hospital protocols for cleaning and disinfecting. And in recent years, many hospitals have chosen more aggressive cleaning agents that may accelerate the wear on their devices. With a bladder scanner that incorporates consumer components, the owner may have to compromise on cleaning and disinfecting to protect their equipment from damage — which could also mean they end up compromising on infection control.
Here is another area where owners of systems that include consumer components can really struggle. A bladder scanner lives in the hectic world of the hospital corridor. They are pooled between users and wrangled by multiple users whenever and wherever needed. That means, in the course of a normal day, a bladder scanner is pulled, pushed, bumped, and may even be misplaced, not to mention cables twisted and probes dropped.
Purpose-built medical devices are designed to withstand the daily onslaught of rough usage and disinfection. Devices like a smartphone or consumer tablet computer are rarely designed to handle that. But some bladder scanner manufacturers want to give the impression that the consumer devices they incorporate are robust enough for a hospital. That is a myth. The latest technology just may not survive the life of a bladder scanner.
Myth #3:
Accuracy Is an Easy Number

The most critical specification for a bladder scanner is the accuracy range. The tighter the range of the device, the more confident you can be in the measurement and subsequent clinical decision you make based on that number.
Q. How much measurement uncertainty is there between a scanner with ± 15% accuracy and a modern scanner that has twice the precision?
A. Measuring a bladder with 500 mL actual urine volume, a scanner with ± 15% accuracy specification has an uncertainty of 150 mL (5.1 fl oz). With a scanner featuring ± 7.5% accuracy, your measurement uncertainty is only 75 mL (2.5 fl oz).
What if two devices claim the same accuracy specification? Then can’t I be equally certain in the measurements?
That is the myth because the human variables are unpredictable.
Compensating for the Human Variables: The Patient and the Clinical Staff
You have no control over what patient will walk through your hospital door. Patients differ in age, gender, anatomy, BMI, medical history, and presenting condition. Some of today’s bladder scanners can automatically compensate for many of these uncontrollable patient variables.
Likewise, your clinical staff has a varied level of skill, training, and familiarity with the technology. High turnover rates are a reality. How does your organization protect itself from the uncertainty of these human factors?
With the right technology and smart device features, today’s scanners can reduce the process to a simple “point and click” operation.
Step 1 / Start
Older devices require an operator to configure a patient type (male, female, child) before scanning. Today’s scanners eliminate this step, saving time and reducing the chance of human error.
Step 2 / Aim
Today’s scanners show onscreen aiming guides that clearly outline the bladder as you position the ultrasound probe allowing you to quickly and confidently find the bladder on all types of patients.
Step 3 / Hold
Once the user indicates he or she has found the bladder, scanners that feature 3D technology automatically take the multiple images required to calculate the bladder volume, resulting in greater user consistency and confidence. Unlike traditional ultrasound, 3D bladder scanners eliminate hand motion and fanning of the probe. The user simply holds the probe in position while the 3D scanner takes a few seconds to do the work.
Step 4 / Review
After the scan, the scanner will provide onscreen feedback to confirm the device was able to see the entire bladder, without any interference from anatomy, such as the pubic bone. The scanner may also alert the user that redoing the scan may lead to a more accurate measurement.
Myth #4:
Artificial Intelligence Replaces Skill
Artificial Intelligence (AI) is becoming widespread in healthcare, reinventing how work is done and how decisions are made. A few bladder scanner vendors now offer devices that boast AI technology. Does that mean that user skill and experience no longer matter?
There are different branches of AI science and the most important for bladder scanners is the recent advancement called “deep learning”. Deep learning is a sophisticated form of AI that is able to learn from large sets of data in order to make predictions. Its advantage over previous AI generations is that deep learning is more robust to natural variations in data and can make conclusions about new data based on previous learning.
Here’s How Deep Learning Works in Bladder Scanners
During the development of a new bladder scanner, the vendor feeds the machine thousands of ultrasound images. As the machine analyzes each image, it makes a conclusion about the characteristics of that bladder — and about bladders in general. Then an expert human sonographer analyzes the same image and tells the machine if its conclusion was accurate. Like a human, the machine learns from experience both by its successes and its mistakes. The important thing to know is that all of this training happens before the device ever ships from the factory. When it arrives on the hospital floor, the machine can apply that built-in knowledge to the new situation of measuring a bladder it hasn’t previously seen. That’s the power of deep learning.
Sometimes it sounds like AI has made the devices so smart that nothing else matters. Here’s where you can separate the AI hype from the AI reality. Compare the critical specifications like accuracy range between AI-assisted devices. Despite some vendor claims about AI, the proof is often in the numbers. What is the benefit of AI if it doesn’t improve accuracy or consistency of results?
The variables of the patient and the clinical staff are ever changing. While AI can compensate for many of these human variables, a truly “smart” solution also combines device ease-of-use, comfort, and workflow simplicity to enable users to harness the promise of AI. Think of an AI-assisted device as a smart companion. The best way to understand AI is simply to watch it in action—in your care environment, with your staff, and your patients.

Myth #5:
I’m Worry Free With a Warranty

Warranty is extremely important. That’s clear. Not only does a good standard warranty indicate the vendor’s commitment to stand behind the quality of its product, but it also removes your uncertainty about future financial impact for repair. But warranty alone doesn’t cover the “soft costs” to an organization for the everyday accidents that will happen to a bladder scanner in the rough and tumble hospital hallway. Downtime and lack of equipment availability ultimately affects patient care. And a warranty doesn’t cover the lost time of staff identifying a damaged device, locating it, contacting the manufacturer, and arranging logistics for the repair.
Talk to your vendor about repair turnaround times, next-day equipment loaner programs, customer support, and repair tracking. Self-repair training programs and built-in diagnostics software can empower Clinical Engineering in its efforts to contain service costs and maximize uptime. And don’t forget to evaluate the vendor’s ability to provide onsite staff training and coaching. These areas are where some vendors truly stand out from the crowd.
When considering a new purchase, look beyond the device itself. Look for a vendor that believes in becoming a true partner in your medical practice.
___________________________________
Brought to You by Verathon
Verathon® is a global medical device company dedicated to innovation in two core fields: Bladder Management (BladderScan®) and Respiratory and Surgical Solutions (GlideScope® and BFlex™). Our mission is to provide innovative and specialized medical solutions that empower healthcare providers to improve and extend patients’ lives.
Verathon has long been at the forefront of point-of-care bladder volume measurement, and we continue to be a leader within the space. Over the past 30 years, we have offered a range of enduring solutions engineered to minimize infection, optimize efficiency and reduce cost.
Our latest BladderScan devices, BladderScan i10™ and BladderScan® Prime Plus™, leverages our second-generation artificial intelligence, deep learning platform, ImageSense®. ImageSense enables greater ease-of-use and accuracy by reducing patient and user variables to consistently and efficiently locate the bladder and measure its volume with just the click of a button.
At Verathon, we are deeply invested in the success of our customers, and we look forward to working with you.
Verathon, a subsidiary of Roper Technologies, is headquartered in Bothell, Washington, and has global offices in Canada, Europe, Asia and Australia.
___________________________________
1. Meddings J et al. Reducing unnecessary urinary catheter use and other strategies to prevent catheter-associated urinary tract infection: an integrative review, website https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3960353/. Accessed November 2018.
2. Frequently Asked Questions about Catheter-associated Urinary Tract Infections, Centers for Disease Control and Prevention website https://www.cdc.gov/hai/ca_uti/cauti_faqs.html. Accessed November 2018.
3. Magill S et al. Reduction in the prevalence of healthcare-associated infections in U.S. acute care hospitals, 2015 versus 2011. IDWeek 2017, website: https://idsa.confex.com/idsa/2017/webprogram/Paper63280.html.
4. Healthcare-associated Infections in the United States, 2006-2016: A Story of Progress, Centers for Disease Control and Prevention website https://www.cdc.gov/hai/surveillance/data-reports/data-summary-assessing-progress.html. Accessed November 2018.
5. Clinical Care Improvement Strategies, Preventing Catheter Associated Urinary Tract Infections, 2013 The Joint Commission.
6. Lee E, Malatt C. Making the Hospital Safer for Older Adult Patients: A Focus on the Indwelling Urinary Catheter.Permanente Journal/Winter 2011; vol. 15(1).
7. This includes the micro cost analysis plus 3 extra hospital days. Reference on excess length of stay: Centers for Disease Control and Prevention website https://www.cdc.gov/infectioncontrol/guidelines/CAUTI/index.html. Accessed November 2018.Reference on cost per hospital day: Becker’s Hospital CFO Report website http://www.beckershospitalreview.com/finance/average-cost-per-inpatient-day-across-50-states.html. Accessed November 2018.